Your childhood stress doesn’t just haunt your mind—it rewires your gut for life, triggering digestive chaos that can persist into adulthood.
Quick Take
- Early life stress permanently disrupts the gut-brain axis, leading to lifelong IBS, abdominal pain, constipation, and diarrhea
- NYU researchers combined mouse models with two massive human cohorts (52,000+ children) to pinpoint how stress reshapes digestive function
- Different biological pathways drive different symptoms, opening doors to personalized treatments rather than one-size-fits-all approaches
- Children of mothers with untreated depression face significantly higher digestive disorder risks, including nausea, vomiting, and colic
The Hidden Scar: How Childhood Stress Rewires Your Digestive System
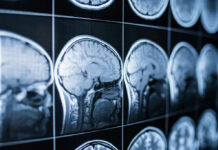
For decades, we’ve known stress damages the mind. But a groundbreaking study published in Gastroenterology reveals stress leaves permanent scars on the gut itself. Researchers at NYU’s Pain Research Center discovered that early life adversity disrupts communication between the brain and digestive system, triggering a cascade of lifelong gastrointestinal problems. This isn’t psychosomatic—it’s biological.
The Evidence: From Mice to Thousands of Children
The research combined animal models with human data spanning over 52,000 children. In mouse studies, newborns separated from mothers developed anxiety, gut pain, and motility problems months later. Female mice developed diarrhea; males experienced constipation. These findings mirrored human outcomes: children exposed to adverse experiences—abuse, neglect, parental mental illness—showed elevated gastrointestinal symptoms at ages nine and ten.
The Mechanism: Sympathetic Nervous System Gone Haywire
The culprit isn’t mysterious. Early stress disrupts the sympathetic nervous system and enteric nervous system—the gut’s “second brain.” This disruption alters how the intestines move food, process pain signals, and maintain barrier function. Kara Margolis, lead researcher, explains: “Understanding the mechanisms involved can help us create more targeted treatments.” The discovery that different biological pathways drive different symptoms—pain versus motility issues—suggests future medications can target specific problems rather than treating all gut disorders identically.
Maternal Depression: An Overlooked Risk Factor
One finding stands out: children of mothers with untreated depression faced substantially higher risks of digestive disorders. These children experienced nausea, vomiting, functional constipation, colic, and IBS at elevated rates. Even more striking, children whose mothers took antidepressants during pregnancy showed increased constipation diagnoses. This suggests prenatal mental health directly influences fetal gut development—a connection most parents and physicians never consider.
Why This Matters Now
Millions of children today experience chronic stress—from pandemic disruptions to economic instability to family trauma. This research reframes unexplained childhood stomach problems: they’re not behavioral quirks or food sensitivities. They’re physiological consequences of stress. Pediatricians can now screen for early adversity when evaluating persistent digestive complaints, potentially preventing decades of suffering and misdiagnosis.
The Path Forward: Personalized Gut Medicine
Rather than prescribing generic acid reducers or motility agents, clinicians will soon target specific pathways. A child with stress-induced pain needs different treatment than one with constipation. This precision approach mirrors modern cancer medicine—tailored to the individual’s biology. The research also validates what many parents intuitively know: a child’s early environment shapes their lifelong health in ways far deeper than we previously understood.
Sources:
Scientists link childhood stress to lifelong digestive issues
Understanding Gut Health and Anxiety in Kids
The Gut-Brain Connection: How Stomach Issues and Trauma Are Linked
Early Life Experience and Gut Microbiome: the Brain-Gut-Microbiota Axis