Five days of binging on junk food can rewire your brain in ways that linger long after you’ve tossed the candy wrappers, triggering metabolic changes once thought to require years of poor eating.
Story Snapshot
- Healthy young men consuming an extra 1,500 calories daily from ultra-processed foods for just five days developed brain insulin resistance and impaired reward learning.
- Brain changes persisted at least one week after returning to normal eating, despite no weight gain occurring during the study period.
- Liver fat increased and cognitive regions like the hippocampus showed reduced insulin sensitivity, mimicking obesity-related metabolic dysfunction.
- The findings challenge assumptions that brain damage from poor diet requires chronic overeating or excess body weight.
Your Brain on a Five-Day Bender
Researchers at Germany’s Helmholtz Center Munich recruited 29 healthy-weight men aged 19 to 27 and split them into two groups. Eighteen participants loaded up on chocolate bars, cookies, crisps, and chips, adding 1,200 to 1,500 extra calories to their daily intake for five consecutive days. The control group stuck to their normal diets. Before the junk food feast began, all participants underwent brain MRI scans and intranasal insulin tests to establish baseline measurements of brain insulin response and reward learning patterns.
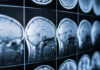
By day six, the damage was already visible. MRI scans revealed increased insulin activity in the brain’s reward regions, elevated liver fat, and a troubling shift in how participants processed rewards and punishments. The junk food group became less responsive to rewards and more sensitive to punishments. This rewiring didn’t vanish when participants resumed healthy eating. One week later, follow-up scans showed persistent reductions in insulin sensitivity within cognitive regions, particularly the hippocampus and fusiform gyrus, areas critical for memory and visual processing.
The Insulin Resistance Nobody Saw Coming
Brain insulin resistance has dominated obesity and diabetes research since the 2000s, but scientists believed it developed slowly alongside expanding waistlines. Insulin normally suppresses appetite and regulates metabolism through brain signaling pathways. When the brain becomes resistant, this communication breaks down, promoting overeating and fat storage. The Helmholtz study upended conventional wisdom by demonstrating that brain insulin resistance can develop independently of body weight or peripheral insulin problems, appearing in lean, healthy individuals after a shockingly brief dietary detour.
The researchers used intranasal insulin delivery and functional MRI technology to isolate brain-specific insulin responses, distinguishing them from the body’s peripheral insulin system measured in standard blood tests. This approach revealed regional vulnerabilities that previous studies missed. The hippocampus, essential for learning and memory formation, proved especially susceptible to junk food’s assault. No changes appeared in the hypothalamus, the brain’s traditional appetite control center, suggesting that ultra-processed foods target different neural pathways than researchers previously suspected.
When Rewards Stop Rewarding
The disruption to reward learning carries ominous implications for long-term eating behavior. Study participants showed diminished responses to positive reinforcement while becoming hypersensitive to negative feedback. This neurological shift creates a perfect storm for unhealthy eating patterns. When the brain’s reward system stops firing properly in response to normal pleasures, individuals often seek more intense stimulation from calorie-dense, ultra-processed foods. The researchers noted this effect essentially primes the brain for obesity, establishing neural patterns that favor continued junk food consumption even after dietary habits improve.
The study’s lead researchers stated that a short-term diet rich in sugar and saturated fat produces prolonged brain effects that outlast the consumption period itself. This persistence distinguishes temporary indulgences from truly harmless dietary deviations. Even occasional binges during holidays or vacations may trigger metabolic changes that resist quick reversal. The one-week follow-up showed effects trending toward baseline but not fully normalized, raising questions about how long complete recovery requires and whether repeated short-term exposures create cumulative damage.
The Ultra-Processed Problem Nobody Wants to Face
Ultra-processed foods now comprise 57 percent of calories consumed in the United States, making this research more than an academic curiosity. The German study builds on a 2019 NIH trial demonstrating that ultra-processed foods drive overconsumption through mechanisms scientists still don’t fully understand. Animal studies have shown that high-fat diets rapidly trigger brain inflammation and cognitive fog, effects now confirmed in humans after remarkably brief exposures. The food industry faces mounting scrutiny as evidence accumulates that these products inflict neurological harm extending beyond simple weight gain or cardiovascular risk.
The economic implications deserve serious consideration. Rising obesity and type 2 diabetes rates already strain healthcare systems globally. If five-day dietary lapses can initiate brain changes that promote metabolic disease, prevention strategies need fundamental rethinking. Current public health messaging focuses on long-term dietary patterns and weight management. This research suggests intervention must address even short-term exposures, particularly in young adults whose brains remain vulnerable to metabolic reprogramming. The social costs of cognitive decline and neurodegeneration add another dimension, especially as researchers investigate Alzheimer’s disease as potential “type 3 diabetes” linked to brain insulin resistance.
The Limitations That Matter
The study examined only young men, excluding women due to hormonal variability that could confound results. Whether females experience similar rapid brain changes remains unknown. Estrogen and progesterone influence insulin sensitivity and reward processing, potentially offering protection or creating different vulnerabilities. The small sample size of 29 participants, while sufficient for detecting the observed effects, limits generalizability across broader populations. Older adults with naturally declining brain insulin sensitivity might prove even more susceptible, or decades of metabolic stability might provide resilience young brains lack.
Some experts offered cautious optimism, suggesting occasional indulgence unlikely causes lasting harm if not habitual. The study’s brief intervention period and young, healthy participants support this interpretation. However, the persistence of effects one week post-intervention and the lack of complete normalization warrant concern. Repeated short-term exposures, common in modern eating patterns alternating between restriction and excess, could accumulate damage that single episodes alone wouldn’t produce. The conservative viewpoint here prioritizes individual responsibility and informed choice. Understanding that even brief dietary lapses carry neurological consequences empowers people to make better decisions, not through government intervention or corporate regulation, but through personal accountability.
Sources:
Just 5 Days of Junk Food Can Trigger Obesity’s Hold on Your Brain
How Just Five Days Of Ultraprocessed Foods Can Disrupt Your Brain
How Just 5 Days of Ultra-Processed Foods Can Impact Your Brain Health