Your brain is lying to you about how much you eat, and it’s doing it on purpose.
Quick Take
- People systematically underestimate their food intake while accurately judging others’ eating habits, revealing a self-serving cognitive bias that protects ego but sabotages health goals
- Three distinct neurological pathways—homeostatic, hedonic, and intentional—compete for control over eating behavior, with biological drives consistently overpowering willpower
- Mindless eating accounts for substantial caloric consumption that occurs entirely outside conscious awareness, driven by environmental cues like plate size and food visibility
- The gut produces 90-95 percent of the body’s serotonin, directly linking dietary choices to mental health, stress levels, and emotional eating patterns
The Perception Gap Nobody Wants to Admit
You finished that bag of chips without realizing it. You ordered a second coffee and a pastry without consciously deciding to. You ate dinner while scrolling through your phone and couldn’t tell anyone what you consumed. This isn’t weakness or lack of attention—it’s your brain operating exactly as evolution designed it to operate, which means it’s operating against your stated health goals.
Research reveals a troubling pattern: people dramatically underestimate their caloric intake while simultaneously overestimating their dietary discipline. More revealing still, this perception gap disappears when judging others. You accurately perceive someone else’s overeating as excessive, yet rationalize your own identical behavior as stress-driven or biologically necessary. This self-serving bias isn’t accidental. It protects self-esteem while preventing the accurate self-assessment necessary for behavioral change.
Three Brain Systems Fighting for Control
Your eating behavior isn’t governed by a single decision-making system. Instead, three competing neurological pathways constantly battle for dominance. Homeostatic eating represents your body’s biological regulation—the system that signals caloric needs through hormonal pathways. Hedonic eating operates through dopamine signaling, the brain’s reward center, which drives consumption for pleasure and emotional regulation rather than nutritional need. Intentional eating represents conscious willpower, the system you believe controls your choices but which is actually the weakest of the three.
The hierarchy matters. Biological drives override intentional willpower almost every time. Stress and fatigue deplete willpower resources, leaving hedonic eating unopposed. Environmental cues—plate size, food visibility, eating location—bypass conscious awareness entirely, triggering consumption before the intentional system even registers what’s happening. Understanding this hierarchy explains why willpower-only diet approaches fail consistently. You’re asking a system designed for short-term decisions to override biological drives engineered over millions of years.
Mindless Eating: The Invisible Consumption Machine
Behavioral economist Brian Wansink’s foundational research demonstrated that people consume significantly more food than they believe they consume. Environmental factors override satiety signals with remarkable efficiency. A larger plate makes portions appear smaller, so you eat more. Food visibility in your kitchen increases consumption by measurable amounts. Eating while distracted—working, watching screens, driving—disconnects eating from conscious awareness entirely. The result: substantial caloric intake occurring completely outside your conscious decision-making process.
This isn’t about willpower failure or moral weakness. It’s about systems operating exactly as designed. Your brain evolved in an environment of food scarcity, where eating whenever food appeared made survival sense. Modern abundance exploits this ancient programming. Food manufacturers engineer products for maximum palatability. Marketing targets psychological vulnerabilities. Environmental design encourages consumption. Your intentional system never stood a chance against this coordinated assault on biological reward pathways.
The Gut-Brain Connection Nobody Expected
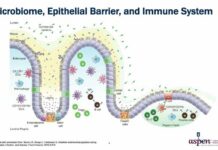
Recent neuroscience reveals an unexpected player in eating behavior: your gastrointestinal tract produces 90-95 percent of your body’s serotonin, the neurotransmitter regulating mood, stress response, and emotional regulation. This means your dietary choices directly influence your mental health and emotional state. Emotional eating isn’t simply about seeking comfort through food—it’s about seeking neurochemical regulation. Stress depletes serotonin, creating genuine biological need for dietary intervention. Your body isn’t malfunctioning when it craves comfort food during stress. It’s attempting self-medication through the most direct pathway available.
This gut-brain axis connection explains why addressing eating behavior requires addressing stress, sleep quality, and emotional factors simultaneously. Willpower approaches that ignore these foundational systems fail because they’re treating symptoms rather than causes. A person experiencing chronic stress with poor sleep has depleted neurochemical resources and weakened impulse control. Telling them to exercise more willpower is neurologically incoherent. Their biology is working against them, not with them.
Social Context: The Hidden Eating Influencer
Research from Cambridge and elsewhere demonstrates that social context—specifically, who you eat with—influences consumption as significantly as what you eat or when you eat. People adjust their eating based on companions’ consumption patterns. Peer influence can increase or decrease intake depending on social comparison dynamics. Eating alone versus in groups produces measurably different consumption patterns. This social dimension of eating behavior explains why restaurant meals exceed home-cooked equivalents and why social eating events produce consumption spikes.
How We Eat vs. How We Think We Eat https://t.co/zC1sXDviJn via @nutrition_facts
— vik wall (@vik_wall393) May 12, 2026
Why Your Brain Judges Others Differently
The most revealing research finding concerns self-other attribution bias. When you overeat, you attribute it to external factors: stress, fatigue, biological need, environmental pressure. When others overeat, you attribute it to internal factors: lack of willpower, poor character, undisciplined choices. This isn’t random inconsistency. It’s a systematic bias protecting self-esteem while enabling harsh judgment of others. The same eating behavior receives entirely different moral interpretations depending on whose behavior you’re observing.
This bias prevents accurate self-assessment. If you consistently attribute your eating to external circumstances, you never develop genuine understanding of your actual eating patterns. You remain convinced your overeating is situational rather than habitual. This cognitive protection mechanism, while psychologically comforting, makes behavior change extraordinarily difficult. Effective intervention requires abandoning this protective bias and developing accurate self-perception—a genuinely uncomfortable psychological process.
The Multi-System Intervention Imperative
Clinical nutrition centers now recognize that single-intervention approaches—diet alone, exercise alone, willpower alone—consistently fail because they address only one of three competing neurological systems. Emerging consensus emphasizes multi-system interventions targeting homeostatic regulation, hedonic reward pathways, and intentional willpower simultaneously. Some approaches include pharmacological interventions targeting dopamine signaling. Others emphasize environmental design changes that support rather than undermine biological drives. Most effective approaches integrate behavioral, psychological, social, and environmental modifications.
The shift from individual blame to systemic understanding represents genuine progress. Eating behavior is multifactorial and complex. Your eating patterns reflect biological inheritance, neurochemical status, environmental design, social context, stress levels, sleep quality, and emotional state—not primarily moral character or willpower capacity. Addressing eating behavior effectively requires addressing these multiple systems simultaneously rather than expecting individual willpower to overcome coordinated biological and environmental opposition.
Sources:
Why do we eat what we eat? – Clinical Nutrition Center
Self-Other Differences in Perceiving Why People Eat What They Eat
How What We Eat Influences How We Feel – Addiction Center